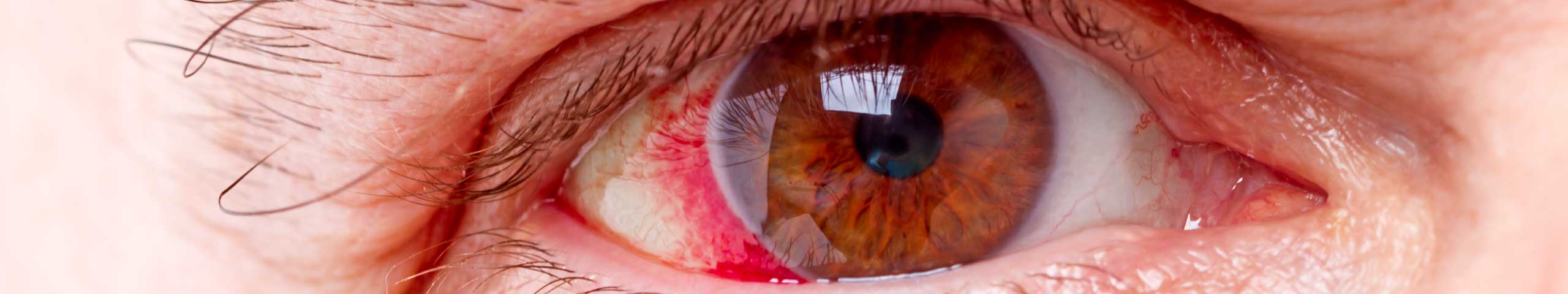
Keratitis is the generic name given to any kind of inflammation of the cornea, the dome shaped translucent membrane at the front of the eye that both covers and protects the eye as well as being part of the focussing function.
The cornea is made up of five individual layers which can all be subject to a variety of inflammations. In the case of Thygeson’s disease it’s the front layer – the epithelial layer – that is subject to the keratitis.
Phillips Thygeson first brought the disease to the attention of ophthalmologists in 1950 from work on his case studies. He defined it as a keratitis where the bouts of inflammation come and go and identified small lesions (punctures, cuts or grazes) on the surface made up of lots of tiny grey coloured dots, together giving a slightly cloudy appearance.
The disease now has been given the official medical name of “Thysgeson’s Superficial Punctate Keratitis” or TSPK.
Although bouts last from several days to a few weeks, returning again within weeks or months, the disease is chronic in that it can last for anything upwards of thirty years. In between bouts the eyes are fortunately normal.
What are the symptoms?
Symptoms are consistent with those for any keratitis:
• Dry and excessively watering eyes at varied times
• Sensitivity to light and glare
• Blurred vision
• The feeling of dirt or grit being in the eye
These symptoms in themselves cannot diagnose TSPK and a slit lamp test is required to provide confirmation by presence of the lesions and minute punctures. Whilst the lesions can cover the whole cornea, generally they seem to be concentrated around the central area.
Who gets it?
The disease is not infectious and quite rare; there is no information on whether or not gender, race or geographic location has any anything to do with it.
Causes of the disease are also somewhat vague, with various viral agents being considered, including the herpes simplex virus, but research is not conclusive.
It’s thought that TSPK might be associated with a variety of actions and conditions:
• Injuries due to arc welding overuse of lamps
• Exposure to chemicals
• Reactions to drugs prescribed for unrelated disorders
• Immune or allergic reaction
Treatment
Eye drops used to act as artificial tears help lubricate the eye and prevent any bumps on the epithelial surface from causing pain and discomfort
Both antiviral and antibiotic medications have proven to be of little use.
Corticosteroids are often prescribed, but careful management of those drugs needs to be carried out in case they prolong the overall chronic nature of the disease. The fact that some immediate relief is obtained from corticosteroid use is indicative that an auto-immune deficiency of some kind is at work.
Soft contact lenses have been found to provide long term relief by comforting the punctures during blinking, but care and discipline with hygiene is essential, otherwise an alternative keratitis – microbial keratitis – may develop.
Refractive and laser surgery has been used to alleviate symptoms but there is little information available on success or otherwise.












Thygeson’s SPK – Personal Success Story
I would like to describe a few steps that I take to significantly reduce my Thygeson symptoms. What I describe here has been very successful for me. Hopefully it works for others too. I just want to share this because I would have loved to have read something like this during the years I was trying to find a way to manage my Thygeson’s.
I have had Thygeson’s keratitis for many years. It used to flare up once or twice a year, and I would go to my eye doctor to get a steroid drop prescription. After a couple weeks of mild steroid drop use per my doctor’s directions my symptoms would go away. Upon the next flare-up I would repeat the cycle.
I never liked the idea of using the steroid drops because supposedly they increase one’s risk of developing glaucoma and other eye issues. A couple years ago my flare-ups became more frequent. Instead of having to go on drops once or twice a year, I was having symptoms every two or three months! Using the steroid drops this often made me very uneasy.
Thankfully, I finally figured out a combination of precautionary measures that I can take to keep my eyes from flaring up. Since adopting these 3 steps over a year ago, I have not had a single flare-up. After years of testing out various hypotheses about what was causing my flare-ups, I finally developed these three rules for myself:
(1) No caffeine
(2) 7 or 8 hours of sleep per night
(3) Use over-the-counter lubricating eye drops
Regarding Points 1 and 2: Years ago, I thought stress and lack of sleep were the primary causes of my reoccurrences. I thought if I just got enough sleep and remembered to stay calm I could avoid flare-ups. But as I mentioned above, a couple years ago my flare-ups started increasing in frequency, sometimes even after periods of good sleep and low anxiety. I was beginning to despair. Then something donned on me. I realized I had been drinking more coffee that year. Originally I thought that primarily lack of sleep and extra stress were causing my Thygeson’s symptoms to worsen. But one day it struck me that less sleep meant I was drinking more coffee. I thought about my last few eye flare-ups and remembered they all came after periods of increased caffeine consumption. I hadn’t been particularly under-slept during some of those periods, but I had been drinking coffee more frequently.
So about a year ago I cut out caffeine completely. No coffee, no tea. And I haven’t had a flare-up since. Cutting coffee may sound difficult, but it’s a price I’m glad to pay to avoid the agonizing pain of a Thygeson’s flare-up.
And to be on the safe side I still try to get enough sleep and remember to breathe when I’m feeling stressed.
Regarding Point 3: If I suspect even the slightest hint of irritation or even the smallest grainy sensation in my eyes I start using over-the-counter lubricating eye drops a couple times a day for a few days. I prefer to use “dry eye therapy” by the brand Thera Tears. I’m sure there are other brands that work too. Even when my eyes feel completely fine, I still use these drops every other night or so. I have also had one or two near-flare-ups, and in those instances I use these drops several times a day for a couple days. It really seems to work.
So by following my three rules, I have been fortunate enough to avoid another flare-up. (1) NO CAFFEINE, (2) GET A FULL NIGHT’S SLEEP, (3) USE OVER-THE-COUNTER EYE DROPS.
Hopefully this helps others out there like me. Let me know if it works for others. I would love to compile more anecdotal evidence about my personal symptom prevention protocol.
Hi, just wondering if you’ve experimented with a small amount of caffeine since, to determine whether it is in fact the primary cause?
Gerry it is possible that caffeine is the trigger for Kirk’s Thygensons. The problem is he is a unique individual like all of us. The old cliche “your poison is my medicine” applies here. Thygeson’s keratitis is not very common yet caffeine consumption is massive globally. Specifically for Kirk, he would need keep getting sleep and use the Thera Tears as he does not and then reintroduce coffee again. Another eye condition that this can be confused with is recurrent corneal erosion. This condition occurs due to dehydrated dry eyes. Caffeine is a duretic, getting more sleep and using Thera Tears of course rehydrates the surface of the eyes, so I wonder if Kirk Mason has had that ruled out?
I have not had recurrent corneal erosion ruled out. Next time I go to the eye doctor I will try to remember to ask. I will say that I have been to 4 different eye doctors, and after thorough examination they have all diagnosed it as Thygeson’s SPK. But I can see how the fact that cutting out a diuretic (caffeine) and using eye lubricating drops is effective for me might suggest the possibility of another condition.
I too suffer from Thygeson’s disease. It has been recurring for about 15 years for me. My flare ups would seem to occur if I had lots of stress in my life. So I too would try ways to relax and reduce stress. Yoga and meditation helps me personally. I recently had eye surgery (removal of corneal lessions) one eye at a time. It was painful and a quick surgery, but it cleared me vision and relieved the Thygeson symptoms. Unfortunately, within 3 months of the surgeries, Thygeson’s corneal lesions grew back. So I am taking prednisone eye drops and tapering them off. I see my doctor in 2 weeks to see how many have grown back. I am discouraged, but strong and will continue to fight and make the best of my situation.
Annika this is a tough situation. I assume you are seeing a corneal specialist?
I have had Thygeson’s for 40 years. I’ve been to MANY opthalmologists including corneal specialist/professors. The best treatment for me has been Long Wear Soft Contact Lenses. I have yet to find anyone to try cyclosporine, but I’d be willing. I’m 60 now, and this year has been a really rough year for me; it’s almost like it was when I was diagnosed at the age of 19. Good luck to you all.
I find it hard to beleive that no one would try cyclosporine for this condition. There is very little downside. It makes sense that long term wear contact lenses help as they bandage and protect the cornea. Cyclosporine is definitely worth trying.
I’ve had Thygensons for about 10 years now and my eye specialist always just prescribed steroid drops when I have a flare up. They don’t seem to even work anymore.
Has anyone had success with Cyclosporine?
I’ve been suffering from Thygensons for about 8 years. My initial doctor got me on cmvarious corticosteroid drops and they would work but I started to get worried being on them so often. He just kept prescribing them so I’ve looked for a different doctor. He has got me on Cyclosporine. I’ve been on it for about a month and unfortunately the condition isn’t any better. I’m seeing the dr again tomorrow. We’ll see 🙏🏼
Hello Stuart,
It is possible to compound the cyclosporine up to 0.5%. Typically the cyclosporine prescribed is only 0.1%
I was diagnosed with Thygeson’s. I was prescribed steroid drops. My eyes cleared up but 3 weeks later I was back to the doctor. This went on for about 20 years. It was a vicious cycle. My eyes were so dry so I began using tear drops. My doctor suggested Refresh Liquigel. It is a very thick gel but very soothing to the eye. Because it’s so thick it blurs your vision and takes 10-15 minutes for eye vision to become clear. My doctor said he never had a patient with Thygeson’s that lasted so long. During one visit he recommended that I try Restasis for my dry eyes. I continued to have regular doctor visits and at one of the doctor visits a couple of years after being on Restasis my doctor commented to me that I have not had one Thygeson’s outbreak since being on Restasis. He wondered whether Restasis cured my Thygeson’s. It’s been about 10 years since I have been on Restasis and not one Thygeson’s outbreak.
Amy this is tricky to know. Thygesons usually eventually clears up. One thing is for sure Restasis is safer than using steroids ongoing.