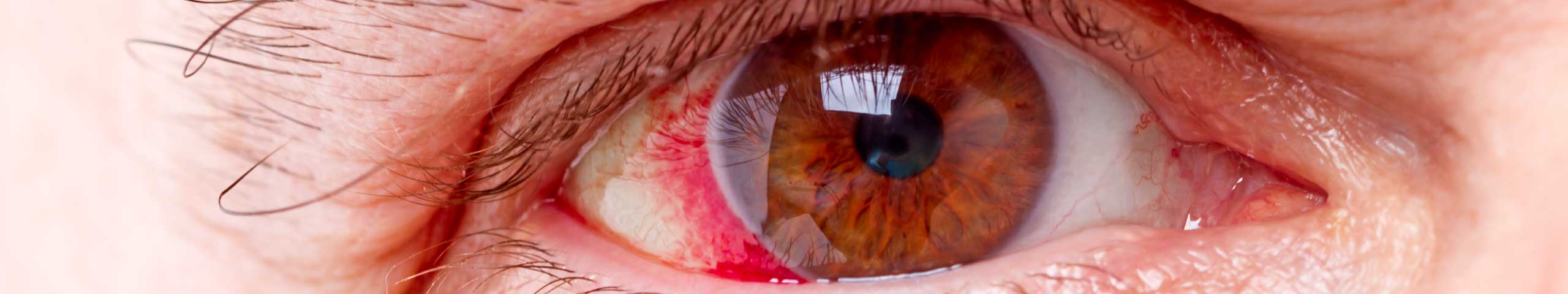
Red eyes are a major complaint in today’s society. Eyes become red for numerous reasons including dryness, exposure to the elements, and air conditioning to name a few. Red eyes are often associated with pain. Before treating, we MUST determine what is causing the redness.
What causes red eyes?
The following list covers many of the possible causes:
Infection
Bacterial infection accounts for a tiny proportion of red eye causes, and yet an antibiotic called Chlorsig is the most frequently prescribed eye drop for red eyes. Chlorsig can do more harm than good if your red eyes are caused by anything other than non-contact lens related bacterial infection. The following is a list of the various bacterial infections in and around the eye that can lead to red eyes.
• Bacterial conjunctivitis
• Viral keratoconjunctivitis
• Blepharitis
• Chalazion
• Stye (hordeolum)
• Bacterial corneal ulcer
• Herpes simplex keratitis
• Fungal keratitis
• Chlamydial conjunctivitis
• Post-operative endophthalmitis
• Pre-septal cellulitis
• Orbital cellulitis
• Dacryocystitis
Allergy
All of the following variants of conjunctivitis are covered in more detail on our
conjunctivitis page.
• Allergic conjunctivitis
• Vernal kerato-conjunctivitis
• Giant Papillary Conjunctivitis
Inflammation
Managing inflammation effectively is key to successful treatment of red eyes. Inflammation is the principle mechanism at work in the following eye diseases:
•
Dry eye syndrome
• Pterygium
• Episcleritis / Scleritis
• Iritis / Uveitis
• Contact-lens acute red eye
• Corneal graft rejection
Trauma
Any ocular trauma, from exposure to burns to penetrating injury, will cause inflammation and redness.
- Corneal foreign body
- Corneal abrasion
- Penetrating eye injury
- Chemical burn
- Solution toxicity
- Recurrent corneal erosions
- Ectropion / Entropion
Elevated Eye Pressure
A pressure spike within the eye can cause acute glaucoma, which presents as a painful, red and light sensitive eye.
- Angle closure glaucoma
- Pupil-block glaucoma
- Pigment dispersion Syndrome
Vascular causes
This is where the small (or new) blood vessels in and around the eye leak blood into the eye’s tissues. It can be harmless, as in most cases of subconjunctival haemorrhage, or it can be serious and sight-threatening, as in the case of neovascular glaucoma.
Treatment for Red Eyes
Treatment centres on controlling inflammation and getting to the underlying source of the problem.
Treat the infection – but only if there is one
The cast majority of red eyes are not caused by bacterial infection and will not respond to broad-spectrum antibiotic drops (such as chlorsig). Red eyes due to viral conjunctivitis will normally resolve within a week or two without any intervention.
Contact-lens related bacterial infection is an ocular emergency.
If you develop red eyes with a muco-purulent discharge (pus) and you are a contact lens wearer,
do not delay in seeing an optometrist or ophthalmologist. This condition requires powerful antibiotics, sometimes in a hospital environment, in order to control the infection and prevent scarring.
Control the inflammation
Inflammation is controlled in several ways:
- Steroid eye drops (preservative-free is better, as preservatives can contribute to red eyes).
- Non-steroidal anti-inflammatory eye drops (NSAIDs)
- Cold compresses (heat inflames, cold calms)
Control the allergy
Allergies may be seasonal or a reaction to pets, dust etc. Management includes
- Anti-histamine eye drops, such as Patanol and Zaditen (these can exacerbate dry eyes)
- Mast cell stabiliser eye drops (these work in a different way to anti-histamines)
- Steroids can be a great kick-start to anti-allergy therapy
- Cool compresses (especially for seasonal allergies)
Manage the underlying dry eye
If red eyes are as a result of an underlying dry eye problem, steroids may only bring symptomatic relief. Finding the real cause of the dry eyes can be difficult and requires a structured approach to diagnosis and assessment.