Words
Published
Macular degeneration (also called age-related macular degeneration or ARMD) is a progressive degeneration of the macular tissue of the eye, resulting in loss of central vision. Objects become blurred in the central part of your vision, making tasks like driving, reading or any fine work difficult.
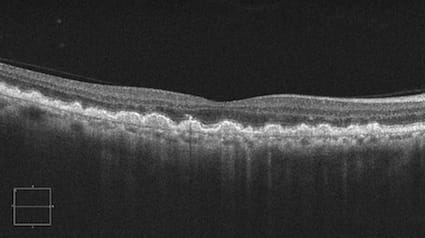 Above: OCT showing dry macular degeneration
Above: OCT showing dry macular degeneration
 Wet ARMD
Up until 10 years ago, the future was bleak if you suffered from wet ARMD. But the arrival of a new group of drugs on the scene over the last decade has changed all that.
Wet macular degeneration occurs because newly formed blood vessels in the eye leak blood into the space underneath your retina. The retina is separated from its underlying support, much like an old-fashioned wall-paper blister pushes the paper away from the wall. New blood vessel growth is a major problem which occurs in a number of eye conditions and usually occurs when that part of the eye is deprived of oxygen. The problem with the new vessels is that they are built very quickly and are faulty. They leak their contents easily into the surrounding tissues.
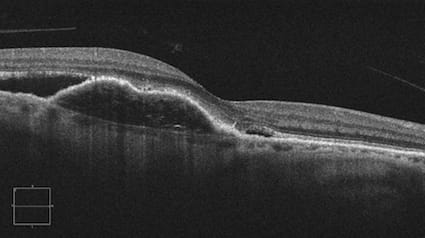
Image right: OCT of wet macular degeneration. The blood can be seen beneath the retina.
Wet ARMD
Up until 10 years ago, the future was bleak if you suffered from wet ARMD. But the arrival of a new group of drugs on the scene over the last decade has changed all that.
Wet macular degeneration occurs because newly formed blood vessels in the eye leak blood into the space underneath your retina. The retina is separated from its underlying support, much like an old-fashioned wall-paper blister pushes the paper away from the wall. New blood vessel growth is a major problem which occurs in a number of eye conditions and usually occurs when that part of the eye is deprived of oxygen. The problem with the new vessels is that they are built very quickly and are faulty. They leak their contents easily into the surrounding tissues.
Image right: OCT of wet macular degeneration. The blood can be seen beneath the retina.
 Do they work?
A number of landmark studies on these drugs found that they effectively halted the progression of macular degeneration in the vast majority of patients and can actually improve the vision in approx. 25-30% of patients. This means, not only does your vision not get any worse, but it may actually get a bit better. The drugs don’t cure ARMD but they can effectively manage it long term and are well tolerated by most patients.
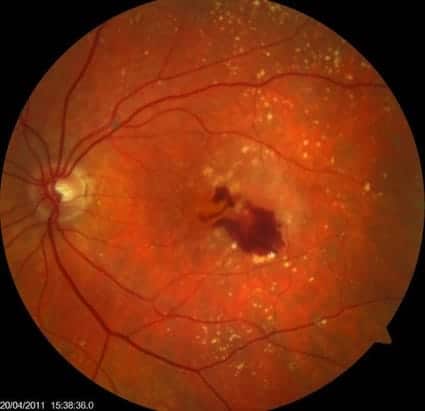
Image right: Wet macular degeneration, showing drusen as well as blood leaking from faulty blood vessels.
Do they work?
A number of landmark studies on these drugs found that they effectively halted the progression of macular degeneration in the vast majority of patients and can actually improve the vision in approx. 25-30% of patients. This means, not only does your vision not get any worse, but it may actually get a bit better. The drugs don’t cure ARMD but they can effectively manage it long term and are well tolerated by most patients.
Image right: Wet macular degeneration, showing drusen as well as blood leaking from faulty blood vessels.
What is Macular Degeneration?
The eye is a bit like a camera, with a focusing system at the front (your cornea and lens) and ‘film’ at the back (your retina). The macula is the central part of the retina, found at the back of the eye, that is responsible for processing central visual images. Right now you are using your macula to read this information. Affecting 1 in 7 people over the age of 50, Macular Degeneration is the leading cause of legal blindness in Australia. You can have the disease in its early stages without knowing. Early detection is vital. If detected early, treatment can be given in an effort to prevent vision loss. Certain changes can even be made to your diet and supplements can be prescribed to support your macula. No time to read the whole article? Download our checklist for macular health here.Types of Macular Degeneration
Dry ARMD occurs 90% of the time in this disease. In this form of the disease, waste products accumulate under the retina, causing yellowish deposits called ‘drusen’. It usually progresses slowly and in most people does not lead to blindness. A minority of people with the dry form can progress to wet ARMD, which accounts for less that 10% of the disease. In this form, the drusen are also present, but so are abnormal blood vessels which leak fluid into the retina. It causes a rapid loss of vision if not treated promptly.Testing for Macular Degeneration
Using the latest in cutting-edge technology, The Eye Practice offers comprehensive screening for this eye disease, which involves three separate tests:- OCT: We are one of very few Optometry practice’s in Australia that screens for Macular Degeneration using Optical Coherence Tomography (OCT), a specially designed instrument that analyses the nerve fibres of the macula for any early sign of disease.
- Retinal Imaging: During your examination, we will also undertake Retinal Imaging, where an image is taken of the macula and then analysed by one of our highly trained optometrists for early signs of the disease. Retinal imaging not only screens for Macular Degeneration it also detects the early signs of glaucoma, cataracts and the eye related effects of diabetes, high blood pressure and high cholesterol.
- Macular Pigment Screening: Our practice was the first in the country to offer MP II macular pigment screening. This non-invasive test takes less than a minute and records a baseline value for your macular pigment. Patients with low levels can begin dietary supplements and lifestyle changes to lower their risk of developing the disease.
 Above: OCT showing dry macular degeneration
Above: OCT showing dry macular degeneration
Causes of Macular Degeneration
No one knows what the exact cause of the disease is. But studies show that it is related to a combination of hereditary and environmental factors. These include smoking and poor diet (see risk factors below).Risk factors
Factors that increase your risk of macular degeneration include:- Age
- Family history and genetics. Researchers have identified several genes that are related to developing the condition.
- Race. This disease is more common in Caucasians.
- Smoking
- Poor diet
- Obesity
- Cardiovascular disease
Treatment for Macular Degeneration
Dry ARMD There is currently no drug to treat dry ARMD (which accounts for 90% of all macular degeneration) but there is a lot of research into finding an effective treatment. Current management centres around identifying patients at risk and using preventative strategies (such as lifestyle factors and supplements) to lower the risk of disease. Wet ARMD
Up until 10 years ago, the future was bleak if you suffered from wet ARMD. But the arrival of a new group of drugs on the scene over the last decade has changed all that.
Wet macular degeneration occurs because newly formed blood vessels in the eye leak blood into the space underneath your retina. The retina is separated from its underlying support, much like an old-fashioned wall-paper blister pushes the paper away from the wall. New blood vessel growth is a major problem which occurs in a number of eye conditions and usually occurs when that part of the eye is deprived of oxygen. The problem with the new vessels is that they are built very quickly and are faulty. They leak their contents easily into the surrounding tissues.
Image right: OCT of wet macular degeneration. The blood can be seen beneath the retina.
Wet ARMD
Up until 10 years ago, the future was bleak if you suffered from wet ARMD. But the arrival of a new group of drugs on the scene over the last decade has changed all that.
Wet macular degeneration occurs because newly formed blood vessels in the eye leak blood into the space underneath your retina. The retina is separated from its underlying support, much like an old-fashioned wall-paper blister pushes the paper away from the wall. New blood vessel growth is a major problem which occurs in a number of eye conditions and usually occurs when that part of the eye is deprived of oxygen. The problem with the new vessels is that they are built very quickly and are faulty. They leak their contents easily into the surrounding tissues.
Image right: OCT of wet macular degeneration. The blood can be seen beneath the retina.
Latest treatment for wet ARMD
Injections of a special type of drug into the eye are the most effective way of stabilising wet macular degeneration. These injections stop abnormal blood vessels from growing and prevent fluid leakage, haemorrhage and scarring of the retina. Like all medications, it wears off and therefore, needs to be repeated regularly to prevent the eye from becoming blind. This is the only treatment that has been proven to stabilise vision loss in patients with wet macular degeneration.Anti-VEGF stands for ‘anti vascular endothelial growth factor’. ‘Anti’ means against, and ‘vascular’ relates to blood vessels. These drugs work by preventing the action of a protein called vascular endothelial growth factor (VEGF) produced by cells in the retina. The original Anti VEGF drug, Avastin, was developed by doctors working on treatments for bowel cancer tumours. (Tumours need a blood supply to feed them and so they create their own new blood vessels). It is still used in the treatment of ARMD, but has largely been replaced by newer versions of the drug called Lucentis and Eyelea. Do they work?
A number of landmark studies on these drugs found that they effectively halted the progression of macular degeneration in the vast majority of patients and can actually improve the vision in approx. 25-30% of patients. This means, not only does your vision not get any worse, but it may actually get a bit better. The drugs don’t cure ARMD but they can effectively manage it long term and are well tolerated by most patients.
Image right: Wet macular degeneration, showing drusen as well as blood leaking from faulty blood vessels.
Do they work?
A number of landmark studies on these drugs found that they effectively halted the progression of macular degeneration in the vast majority of patients and can actually improve the vision in approx. 25-30% of patients. This means, not only does your vision not get any worse, but it may actually get a bit better. The drugs don’t cure ARMD but they can effectively manage it long term and are well tolerated by most patients.
Image right: Wet macular degeneration, showing drusen as well as blood leaking from faulty blood vessels.
Lucentis and Eyelea injections
Eye drops and oral medications just don’t deliver enough of some drugs to the retina to be effective. An injection is a safe and efficient way to get the drugs to where they are needed.- These drugs are injected into the eyes at intervals of about 4 to 6 weeks. If that sounds like an ordeal, it may be helpful to know that almost every patient feels like that at first but the reality is usually much better than the idea of it.
- The eye is numbed with eye drops, so you don’t feel pain (but you usually feel some pressure). Usually you won’t even see the tiny needle used to inject the drug through the white of your eye (the sclera). The most common sensation is a burning sensation related to how the eye is prepared for the injection (using antiseptic).
- The site of the injection can be a little tender for a day or two afterwards. Risk of complications is very low and will be discussed by your surgeon.
- Your retinal doctor will get you to return every 4 to 6 weeks at first and may schedule some breaks in the treatment, depending on how you are responding.
- This treatment only works on active disease – that is where there is some leakage from blood vessels actually occurring. It is not effective on damage that occurred years ago. If your optometrist diagnoses wet ARMD in your eyes, it is essential to see a retinal specialist promptly for treatment.
- Researchers are working on a way for an implant to slow-release these drugs within the eye over a period of years. This is good news for needle-phobic patients with macular disease!
Other surgical treatments for ARMD
These have largely been superseded by injections of Eyelea and Lucentis, and are rarely used now: Photo-dynamic laser therapy A drug is injected into your blood stream and gets absorbed by the abnormal blood vessel of your retina. A special laser can then target these vessels and destroy them. Retinal translocation If the problematic blood vessels are right under your macula, the surgeon can’t safely treat that area with a laser because of the likely damage to your retina. In this case, the surgeon may rotate the macula away from the underlying blood vessels, which may then be treated.Low vision aids
If you have permanent damage to your vision due to ARMD, you may need the support of low vision aids. These are usually specially designed magnifiers (often in combination with powerful lights) and can significantly improve your ability to read and maintain your independence. Specialist optometrists can find the best low vision aid for you. If your own optometrist doesn’t supply them, they can refer you to somewhere that can.Prevention of macular degeneration
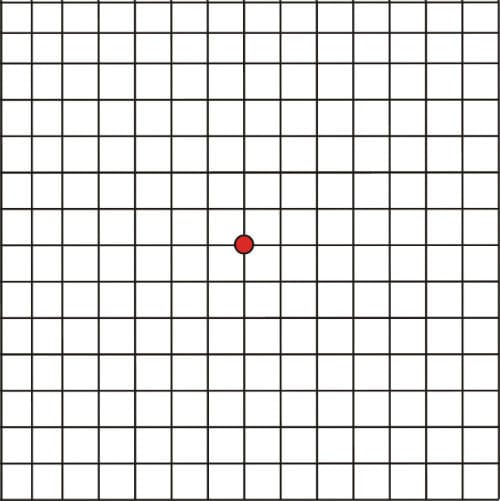
The earlier you get a diagnosis of AMD, the greater the chance that treatment will help. See your eye doctor if you have any symptoms of AMD, and make sure you keep a regular schedule of eye exams. Try these prevention tips:- Check your sight regularly by looking at an Amsler grid – a pattern of straight lines that’s like a checkerboard. It can help you spot changes in your vision. To do this, cover one eye and look at the black spot in the centre of the grid. The lines should appear straight and unbroken. Inform your optometrist if you notice that the lines are wavy or broken.
- If possible, stop smoking.
- Eat a balanced diet that includes leafy green vegetables (especially kale).
- Protect your eyes with sunglasses that block harmful ultraviolet (UV) rays and blue blockers that protect your eyes from the harmful effects of computer-emitted blue light.
- Supplements with antioxidants plus zinc (such as Macutec) may lower your odds of getting AMD, according to the Age-Related Eye Disease Study. Talk to your optometrist if you have a family history of macular degeneration.
- If you’re over 55, your vision exams should include testing for ARMD.

Don’t risk damage to your eyesight. Phone The Eye Practice today to arrange an eye exam on (02) 9290 1899 or request an appointment online.
Comments
Free resources
Sign up
Latest news





