‘What’s the best treatment for my red eyes?’ is a question we get practically on a daily basis at The Eye Practice in Sydney’s CBD. Many of our patients suffer from dry eyes and redness is one of the symptoms that causes them most concern.
They often don’t realise that use of decongestant drops such as Visine can actually cause red eyes rather than cure them.
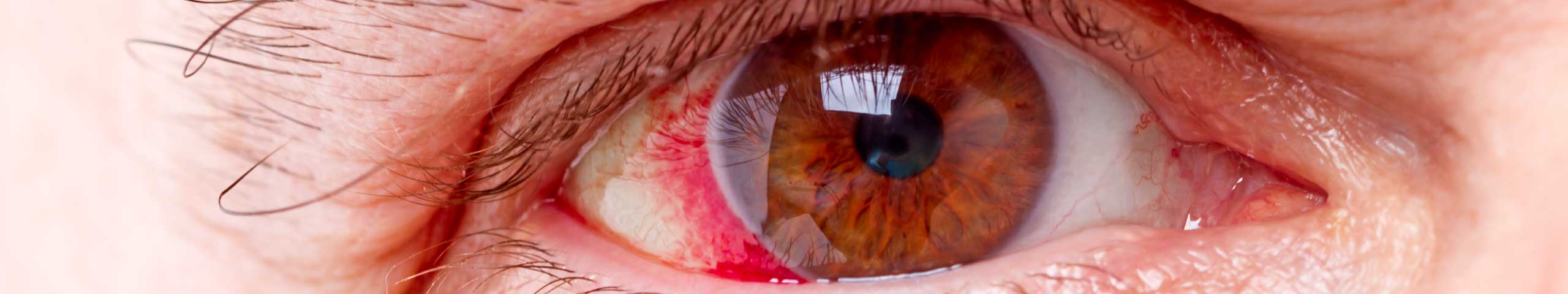
What causes red eyes?
Redness is caused by inflammation of the blood vessels of the conjunctiva (conjunctivitis) and the sclera (the white of the eye). This inflammation is often secondary to a range of underlying eye problems including infection, allergy and dryness. Getting to the root cause of the inflammation will yield far better results than simply attacking the inflammation itself with decongestant drops such as Visine and Clear Eyes, which constrict the blood vessels and provide no therapeutic effect. These drops are also called vaso-constrictors. Decongestants only work as long as you are using them and are commonly associated with rebound redness, where the blood vessels become inflamed again as soon as you stop taking the drops. This is how people get hooked on decongestants – not just eye drops but also nasal sprays. The other problem with decongestant eye drops is that they are usually preserved with BAK, a preservative that is toxic to the delicate tissues of the eye and can in itself lead to further redness.
Should eye inflammation ever be medically treated?
Yes, absolutely, as long as the underlying cause of the inflammation is being treated. Some inflammatory conditions affecting the conjunctiva or white of your eye, as well as dry eyes, respond very well to topical steroid drops prescribed by a therapeutically-endorsed optometrist (or an ophthalmologist).
What is the alternative to decongestant eye drops like Visine?
Steroid eye drops are the most effective treatment for inflammation. Patients are often a bit funny about steroids; they tend to think of them as powerful – even dangerous – drugs, when in fact they are some of the most effective eye drops for clearing up red eyes. Milder steroids such as FML are gentle on eyes but very effective against inflammation. They must be prescribed with confidence and used according to the directions. The worst thing you can do with steroids is to use them less often or for a shorter duration than prescribed. This is a common scenario: The eyes start to get better and become whiter; the patient decides to stop taking the steroid eye drops and, BAM! you’re right back where you started with your red eye. At their most effective, steroids are used aggressively – stronger and longer than you think is necessary. This avoids the rebound redness that can occur if they are discontinued too early. Steroid eye drops are only available on prescription and can cause a temporary increase in intraocular pressure in some patients and so are always used under the supervision of a therapeutically-endorsed optometrist or an ophthalmologist.
What if the inflammation is secondary to another condition?
The best way to rid eyes of redness caused by an underlying condition is to effectively treat that condition. Antibiotics treat eye infections and anti-allergy medications such as anti-histamines treat allergy. Dry eye is a complex ocular condition with a wide range of treatments. All of the above can include an anti-inflammatory eye drop as part of the treatment but not a decongestant! Remember, decongestants don’t treat inflammation – they simply bring about temporary symptomatic relief and often cause worse redness than you started with.
What if I have a pinguecula or a pterygium?
We previously wrote about the difference between pinguecula and pterygium here. If you suffer from one of these conditions, your eyes may be inflamed and red. While pterygium often requires a surgical solution if it starts to encroach onto your cornea, pinguecula is usually managed without surgery. A pinguecula is normally yellowish or clear and may only become inflamed due to a poor-fitting contact lens. Ocular lubricants may be sufficient to reduce the redness. With either condition, if redness is causing you concern, talk to your eye specialist or optometrist about a short course of ocular steroids rather than reaching for the Visine.
In summary, ocular decongestants have very limited use. There are occasional scenarios when they can be useful – such as a one-off photo shoot or special occasion (such as a wedding) where you have developed some ocular redness just beforehand and want to limit the redness for that specific event. But bear in mind that their use will almost certainly result in even redder eyes the following day and that to continue using the drops can get you hooked!