Yes !
Advances in the manufacture and properties of contact lenses mean that today wearers have three basic decisions to take:
How often to replace:
- Daily Disposable – new lens used every time
- Disposable – lasting up to two weeks
- Frequently replaced – up to three months
- Traditional re-usable –replaced after 12 months or so
When to wear:
- Daily – taken out every night
- Extended wear – left in day and night for up to 30 days
Type to use
- Soft, hard (semi-rigid gas permeable), Hybrid (combined soft periphery and rigid centre)
In all of the three choices to be made the matter of risk of corneal neovascularization needs to be addressed.
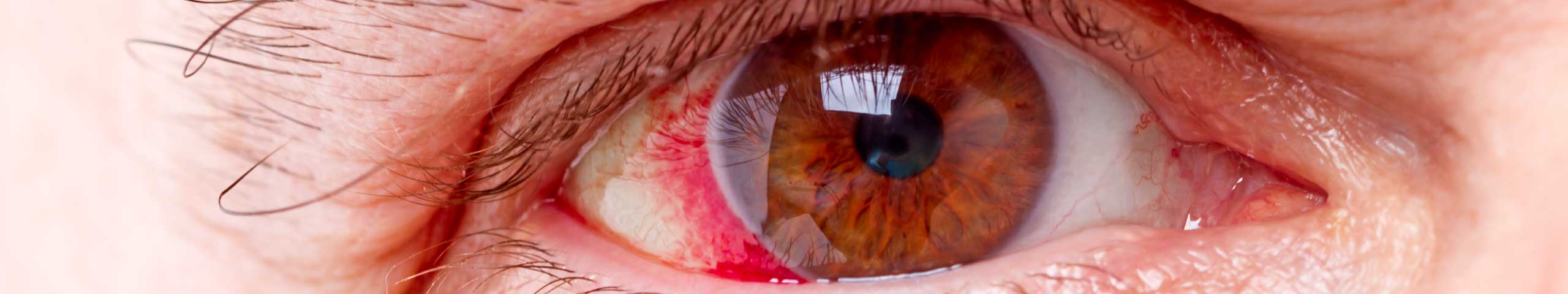
What is corneal neovascularization?
The cornea at the front of the eye is transparent and is a most unusual part of the body since it is “avascular” – that’s to say the opposite of vascular or containing blood vessels.
Blood is needed to carry oxygen throughout the body, and an interesting question then arises – “how does the cornea get its oxygen”. Well, since the cornea is at the front of the eye it is able to absorb the oxygen it needs from the atmosphere.
If new blood vessels begin to develop from the limbus, which is the joint between the cornea and the white of the eye for whatever reason, the condition related to the cornea is called “neovascularization” coming from the Greek word neo meaning new, and the Latin word vasculum meaning blood vessel.
The development of the new blood vessels in the cornea can have some serious consequences:
- If they grow into the cornea enough they can cause irregularity to the cornea, which in turn will degrade the vision.
- In severe cases the cornea will lose its clarity and with further vision degradation only a corneal transplant will clear the vision.
How does it start?
Although caused possibly by an infectious inflammation or an injury, a majority of cases today stem from the inappropriate use of contact lenses.
For a particular person, if the contact lenses are not replaced frequently enough, they are left in at night too much or they are not gas-permeable then the amount of oxygen that can be absorbed is limited. The growth of the new blood vessels is then usually accompanied by inflammation.
Contact lens wearers who frequently take little naps without taking out their lenses and those people who let the required strict hygiene regime slide a little are susceptible to the condition.
A slit lamp test carried out by an optometrist will determine the presence of any corneal neovascularization; corneal sensation measurements help further identify the condition.
What are the symptoms for contact lens wearers?
Contact lens wearers might begin to:
- Feel irritation in the eyes, and some dryness
- Exhibit “pink eye” or conjunctivitis
- Feel somewhat uncomfortable with the lenses near the end of the wearing period
- Often there are NO symptoms.
Treatment
The optometrist who prescribed and fitted the contact lenses will initially adapt one or all of the three elements – replacement, wearing time and type – in order to alleviate the problem.
If the condition is advanced then the wearing of any contact lenses will be suspended for a while and drops applied – directly to the cornea- usually corticosteroids.
If the situation is really severe and corneal scarring and/or vision have been impaired then it may be necessary to carry out a laser procedure, or in the worst case scenario a corneal transplant.
Epilogue
Considering what can happen, it’s obvious that both users and intending users of contact lenses should make sure they follow the instructions given by their optometrist or ophthalmologist, and that the eye professionals ensure that their patients receive appropriate follow up consultations.