Glaucoma is a condition that affects the optic nerve of the eye to such an extent that all vision can be lost, since it is the optic nerve that sends the light messages received on the retina at the back of the eye directly to the brain where they are processed.
Glaucoma is a condition that affects the optic nerve of the eye to such an extent that all vision can be lost, since it is the optic nerve that sends the light messages received on the retina at the back of the eye directly to the brain where they are processed.
There are various types of glaucoma with the two main types being described by the way in which the aqueous humour within the eye, just behind the cornea, is prevented from draining naturally through a very fine mesh called the trabecular meshwork and located at the junction of the cornea and iris.
The iris surrounds the lens of the eye, but if the angle at which they touch is wide, then everything is fine. In the closed angle type of glaucoma the iris and the lens come into permanent contact because the angle becomes very acute.
When this happens the trabecular meshwork is effectively closed and since drainage is prevented, the internal eye pressure (intra ocular pressure) increases.
Increase in eye pressure has the unfortunate effect of degeneration of the optic nerve which sends messages received by the retina to the brain.
Who is at risk?
Older people are more at risk, and with the ageing of the population the number of people developing glaucoma is on the increase.
Being long-sighted is a risk, because the long-sighted eye typically is smaller than normal. This in turn means that the drainage system is smaller and is more likely to close.
Most at risk though are Asians. In this population closed-angle glaucoma is the most common form of glaucoma.
A family history of glaucoma is an important indicator. An optometrist questions this during an eye examination with a new patient.
It is considered expedient for all people, even those who have no reading or vision problems whatsoever to undergo an eye examination for the sole purposes of detecting glaucoma – early detection means effective management!
How is closed angle glaucoma detected?
A case of closed angle glaucoma can usually be detected quite simply since blockage of the trabecular meshwork causes several symptoms including pain, and hence a visit to the optometrist or ophthalmologist becomes essential. A series of tests carried out in conjunction with a routine eye examination will indicate the presence of glaucoma.
Symptoms other than pain include:
• Blurred vision
• Occasional headaches accompanied by physical sickness
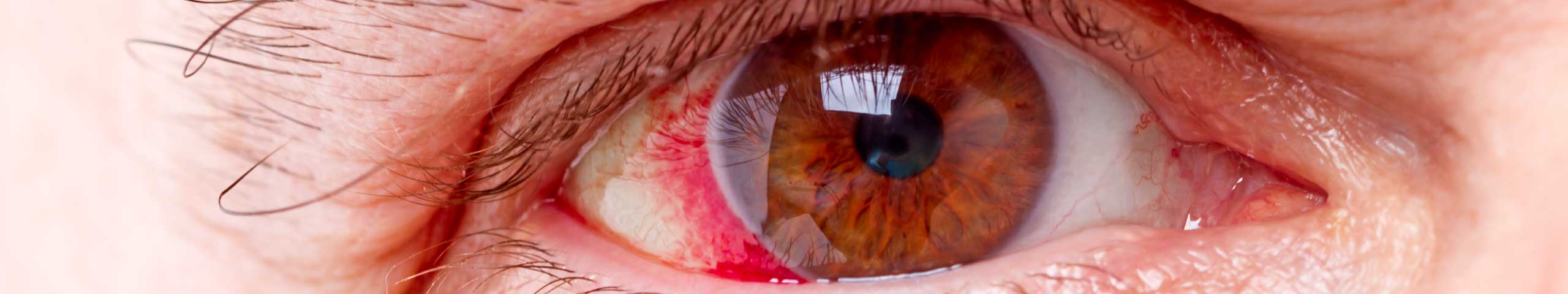
• Redness in the eye
• A halo effect seen around a bright light
• Unfortunately some cases of closed-angle glaucoma are not acute (occur slowly). This means that there are no symptoms. Therefore regular eye examination is the best way to rule out all forms of glaucoma.
If the closed-angle glaucoma is sudden (acute), it is a medical emergency. If the attack is not broken, blindness in the affected eye is likely.
Treatment
In all cases of glaucoma, treatment is administered not to cure the glaucoma but in order to manage and prevent further degeneration and loss of vision.
Once symptoms have been alleviated a positive approach to management is often taken to undo the blockage to the trabecular meshwork through laser surgery, the objective being to open up the angle between iris and lens to prevent contact.
The procedure – called an iridotomy (done by laser) – has a good success rate in cases where the glaucoma is only moderately developed. In some cases an iredectomy might be required which is done with a surgical incision.