About managing keratoconus
Managing keratoconus is complex because the disease changes over time and affects both eyes differently. That said, the treatment often restores good vision. There are two keratoconus main options: non-surgical and surgical.

Non-surgical keratoconus management uses glasses or contact lenses to improve vision. Surgical options include collagen cross linking, the use of Intacs and intraocular contact lenses (ICL) as well as corneal transplants.
The best option will depend on the type of keratoconus a patient suffers and how far the disease has progressed.
Important
It’s important to note that keratoconus management is not a cure. Rather, it aims to restore clear vision.
Non-surgical keratoconus management
In most cases the management for keratoconus will not require surgery. Indeed, eye glasses usually work well in the early stages of the disease. However, as it progresses most sufferers will need contact lenses.
Glasses for keratoconus
In the early stages, glasses can be an excellent option. In fact, people with mild keratoconus can get good vision with an expertly matched prescription from a keratoconus optometrist.
Contact lenses for keratoconus
Contact lenses are the most common keratoconus option. In fact, there are usually five different types of contact lenses that optometrists use in management of the disease.
Surgical keratoconus management
There are five types of surgical keratoconus management. These range from minimally to highly invasive.
Minimally invasive options are common and effective, but more invasive surgical treatment is usually avoided. In fact it is only an option if someones vision has become very bad, or contact lenses have become too uncomfortable.
Corneal collagen cross linking
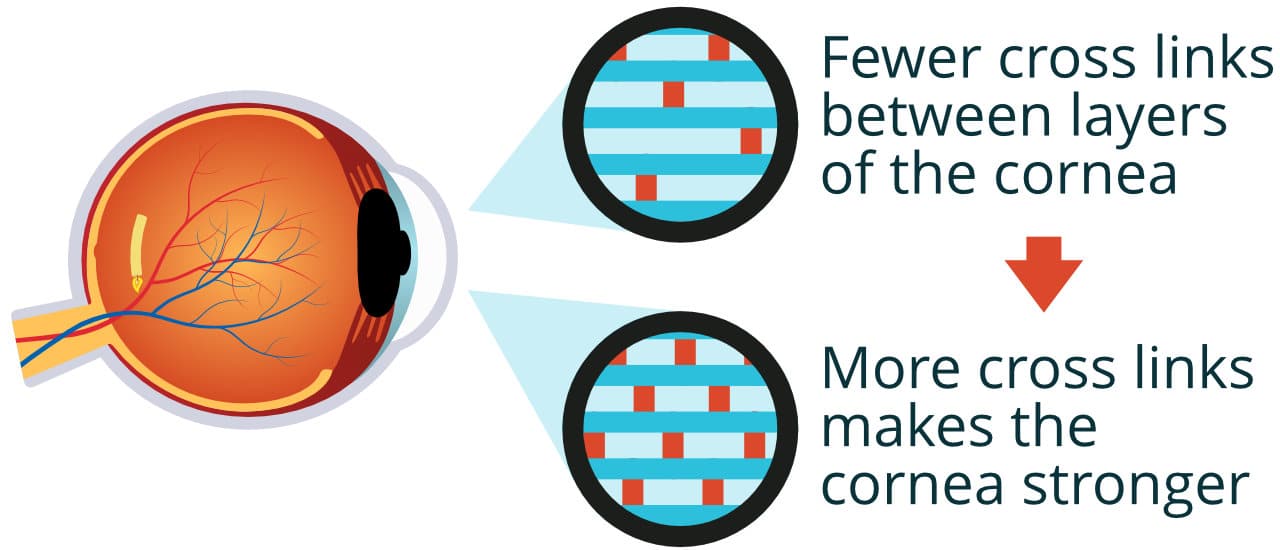
This is a minimally invasive procedure designed to strengthen the cornea. It works best during the early phase of keratoconus and can slow or even stop the misshaping of the cornea.
The procedure works by using specially formulated vitamin B2 eyedrops which – under ultraviolet light – create new, strengthening bonds between collagen fibres in the cornea.
Combined corneal cross linking + laser eye surgery
The aim of this combined procedure is two-fold: Firstly to stabilise the condition and stop keratoconus getting worse; and secondly to reshape the surface of the cornea to improve vision.
Intraocular contact lenses (ICL)
These small, soft contact lenses are surgically inserted inside the eye through a small incision. While intraocular contact lenses can be of benefit to patients who are having difficulty wearing normal contact lenses, the procedure is considered invasive so not used often.
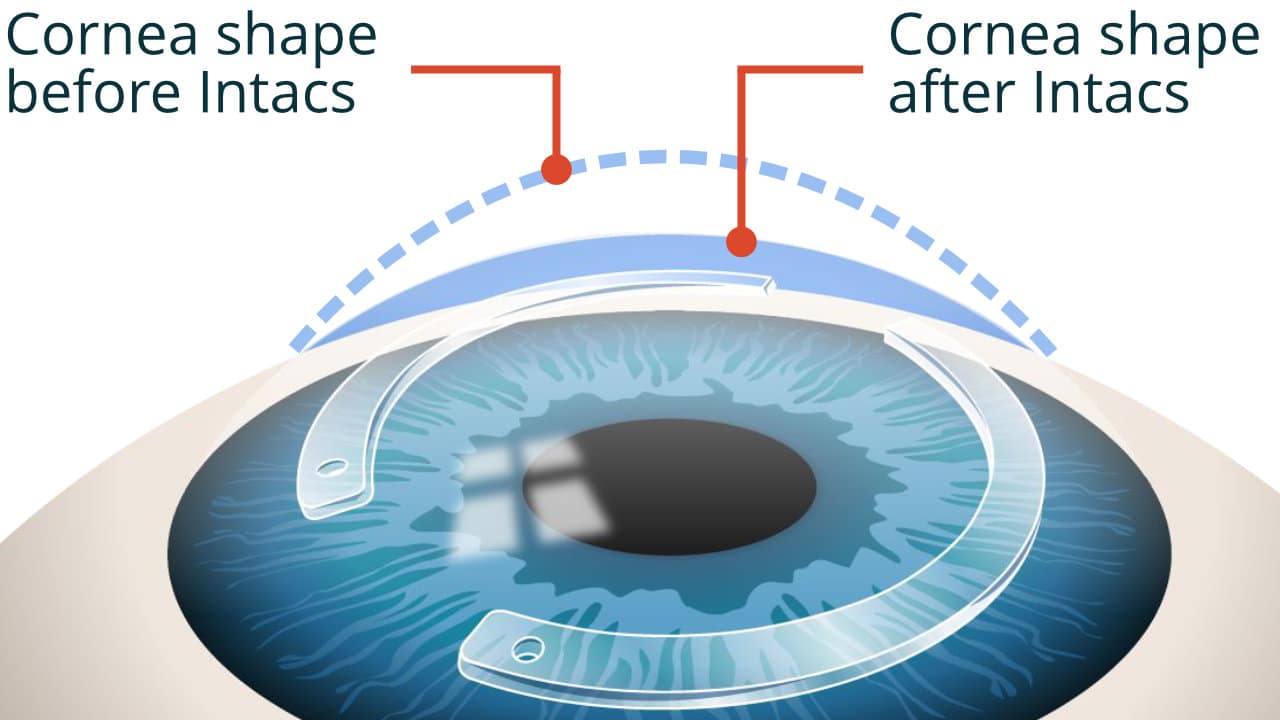
Intacs (intra corneal ring segments)
Intacs are clear implants with an arc-shape. They are surgically positioned into the cornea to reshape the surface of the eye so that vision is improved. However, this minimally invasive surgical procedure hasn’t given reliable results.
Corneal transplant
A corneal transplant is a highly invasive surgical procedure. Indeed, it involves grafting a donated cornea onto a patients own cornea.
However, a corneal transplant does not restore perfect vision. In fact, most patients will still need glasses or contact lenses. Fewer than 5% of people with keratoconus need to get a corneal transplant.
Dr. Jim Kokkinakis can help manage your keratoconus
Dr. Jim Kokkinakis has been managing keratoconus in his patients for decades. In fact, he is one of the foremost keratoconus optometrists in Australia.
Jim is also a Senior Lecturer at the Optometry School UNSW where he teaches on the subject. In addition, Jim is a Fellow of the International Society of Contact Lens Specialists (ISCLS).
Book an appointment to learn more about the best keratoconus treatment for you.



