Pharmacy shelves are packed with a bewildering assortment of drops for dry eyes. Many of these are non-medicated lubricating drops – or artificial tears. But there are several other types of drops, which can be very confusing. The following is a guide to the various types of drops used in the treatment of dry eyes.
Artificial tears
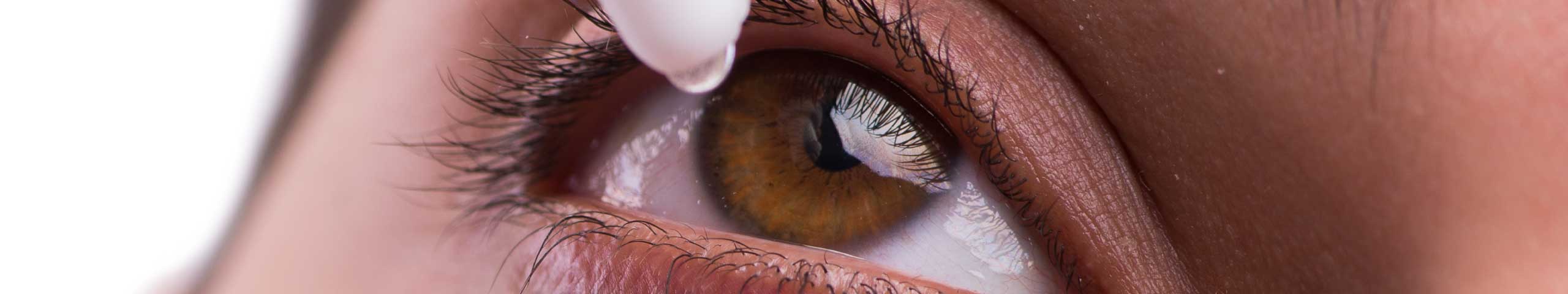
These consist of a huge range of lubricating drops, gels and ointments that supplement your own natural tear film. They come in preserved and unpreserved formulas. Unpreserved eye drops are always recommended (rather than preserved ones) as the perservatives are designed to kill live cells and can be very toxic to the eye’s delicate tissues. Choose unit dose eye drops in small plastic tubes or measured dose eye drops in a valved delivery system (such as Hylo Forte). This avoids adding any additional irritants into your eyes.
Artificial tears have a role in supplementing your natural tear film, particularly in dry environments such as offices and airplanes. They replace moisture stripped by the dry air. In this way they act much like a moisturiser on your skin. We would caution, however, against the overuse of these drops. Even though they are not medicated, they can do more harm than good when overused. If you find you are using them more than 4-6 times a day, and not just in dry environments, then there is likely to be an underlying cause of dryness that is not being addressed. A proper diagnosis of your tear film, blink rate and quality and tear gland function, can help to identify what the underlying problem is.
Decongestant eye drops
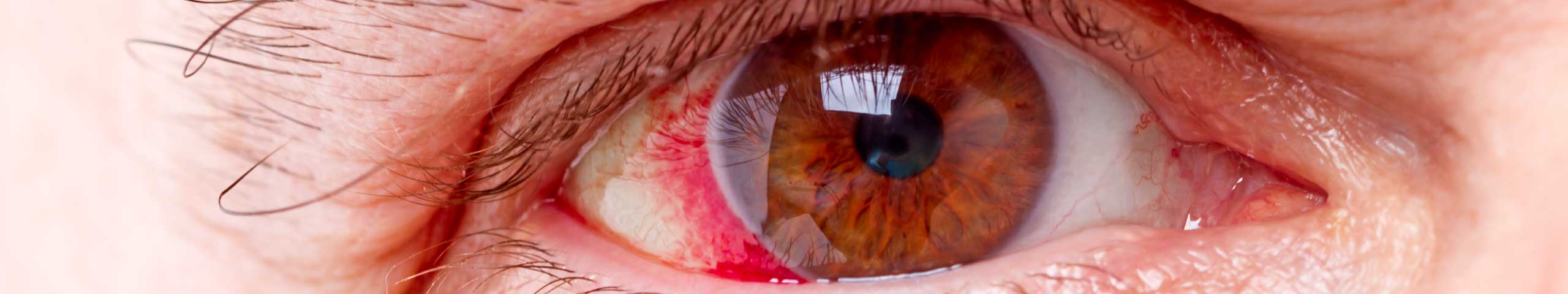
These are vaso-constricters and cause the tiny blood vessels of the white of your eye to shrink, making the eyes look less red. They should be avoided other than for one-off occasions if absolutely necessary, as they result in a rebound effect. This means that when you stop using the eye drop, your eye becomes redder than it was to start. Decongestants are highly addictive. They do not treat the underlying cause of redness or dryness.
Antibiotic eye drops
Most red eyes are not caused by a bacterial eye infection, but when they are, antibiotic eye drops are often prescribed. Antibiotic eye drops are also used after surgery, to protect the vulnerable eye from getting an infection. Antibiotic eye drops are used to treat bacterial conjunctivitis, contact lens related eye infections and bacterial infections that can occur after eye surgery or trauma to the eye. Certain bacterial eye infections are sight-threatening if not treated early and aggressively with antibiotics. These include some contact lens-related eye infections and infections that can occur inside the eye after surgery or injury. The serious eye infections are often treated in hospitals to ensure the best outcome.
One of the most overused eye drops is an antibiotic called Chlorsig. It is indicated for the treatment of bacterial conjunctivitis and other non-sight-threatening eye infections unrelated to contact lens wear. Unfortunately is grossly overused. At the first sign of a red eye or conjunctivitis, GPs and patients reach for the Chlorsig (or Chloramphenicol eye drops). In fact, most of the time, these drops are not indicated and do more harm than good. If you have used them for 7 days and your symptoms have not resolved, then they are not the right drops for you. Stop using them and see a therapeutically endorsed optometrist or ophthalmologist for correct diagnosis of what’s going on. GPs can be the most trigger-happy when it comes to over-prescribing these eye drops.
Steroid eye drops
These are the mainstay of treatment for eye inflammation – whether caused by disease, infection, allergy or dryness. They are also used after eye sugery to control inflammation. Steroid eye drops, and their cousins, the non-steroidal anti-inflammatories (or NSAIDs) come in a range of different strengths, depending on what is being treated. They should always be used for the duration recommended by your doctor / therapeutically endorsed optometrist.
People are often tempted to stop using steroid eye drops as soon as their eyes begin to feel better, but this can quickly result in a rebound effect – and worse inflammation than you started with. Both steroid and non-steroidal eye drops can cause the pressure within your eyes to become raised, and therefore a baseline reading should be taken before you start the drops, and regular pressure checks performed while you are using them. They are generally not used long-term, and usually used for a course of a few weeks.
Antihistamine eye drops
These are used in the management of allergy, when your eyes are itchy, watery and uncomfortable. They prevent the release of histamine by your own body, which causes the itching, redness and watering assoicated with hayfever, seasonal allergies and allergies to pets. Antihistamine eye drops (and tablets) can aggravate dry eyes, so if you suffer from dry eyes, they may not be the best choice for you. Your therapeutically endorsed optometrist may recommend a short course or unpreserved steroid eye drops instead.
Preservatives in eye drops
Unfortunately, most eye drops are preserved. If it comes in a bottle with an opening in the nozzle, it will be preserved. Preservatives are bad news for eyes, especially if you suffer from dry eyes or allergy. Most eye drops are actually available from compounding pharmacies in a non-preserved preparation. This is where The Eye Practice can make a big difference to the management of your dry or red eyes. We liaise with compounding pharmacies to provide preservative-free versions of most eye drops.